

Learn how cortisol and adrenaline affect the metabolism of first responders and veterans, including risks for chronic stress, weight gain, and burnout.
Introduction
First responders and military veterans face intense physical and emotional stress throughout their careers. Whether it’s a high-speed police chase, a structure fire, or combat operations, these stressful situations trigger powerful hormonal responses that prepare the body for survival. Two of the primary stress hormones involved in these life-or-death responses are cortisol and adrenaline (epinephrine).
While these hormones are essential for short-term survival, chronic activation of these systems can damage the body in the long run, disrupting metabolism, immune function, and emotional well-being.
In this post, you’ll learn:
- What cortisol and adrenaline do in the body
- How chronic stress affects metabolism
- Why first responders and veterans are uniquely at risk
- Practical steps to support long-term health
What Is the Stress Response?
The human stress response is a finely tuned survival mechanism. When danger is perceived, the sympathetic nervous system is activated, releasing adrenaline. This causes the classic “fight-or-flight” symptoms:
- Faster heart rate
- Increased breathing
- Redirected blood flow to muscles
At the same time, the hypothalamic-pituitary-adrenal (HPA) axis activates cortisol production, which prolongs the stress response to keep energy available for survival (Herman et al., 2016).
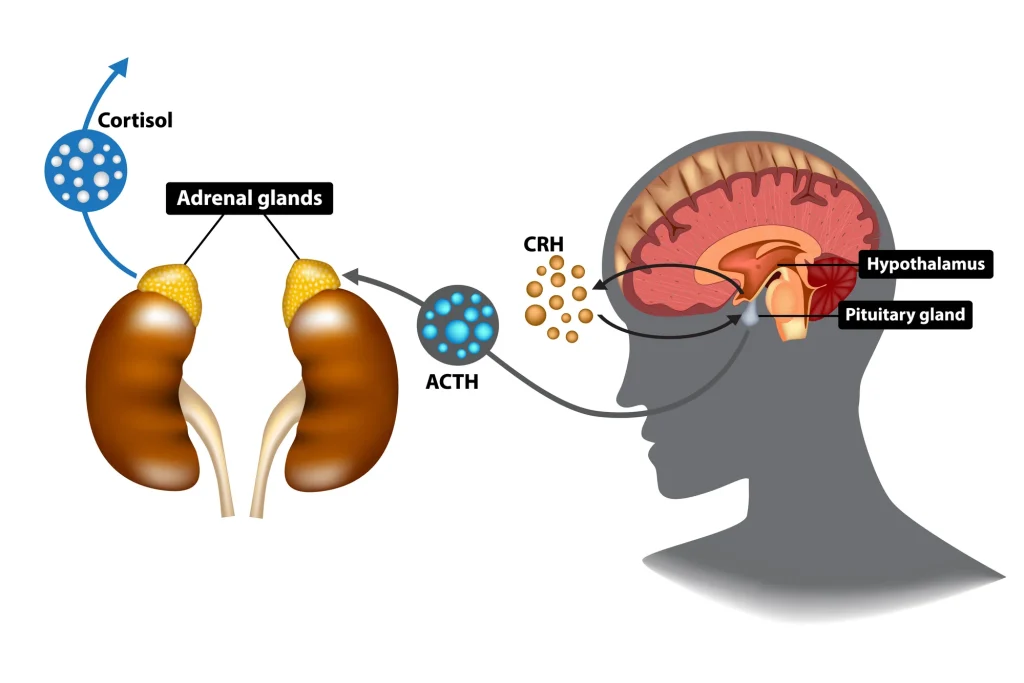
https://www.simplypsychology.org/hypothalamic-pituitary-adrenal-axis.html
Cortisol’s Role in Metabolism
Cortisol is a glucocorticoid hormone whose key role is to maintain blood glucose during stress (Sapolsky, 2004). It does this by:
- Stimulating gluconeogenesis (creating glucose from amino acids)
- Blocking insulin’s effect, which keeps sugar in the blood for muscle use
While this is helpful short-term, chronically high cortisol can have serious health impacts (Yaribeygi et al., 2017), including:
- Abdominal weight gain
- Insulin resistance
- Increased appetite and cravings
- Muscle loss
These effects directly disrupt a person’s metabolism, raising the risk of obesity, diabetes, and heart disease (Rosmond, 2005).
Adrenaline’s Impact on the Body
Adrenaline, or epinephrine, works within seconds. It:
- Raises heart rate
- Opens airways
- Releases glucose from stored glycogen
- Diverts blood flow from digestion toward the muscles
While critical for surviving emergencies, repeated adrenaline surges (such as in firefighting or combat) can lead to:
- High blood pressure
- Chronic anxiety
- Poor sleep patterns (Dimsdale, 2008)

Why First Responders and Veterans Are Uniquely at Risk
First responders and veterans operate in environments of chronic, repeated stress. Common features include:
- Hypervigilance (always scanning for threats)
- Night shifts and circadian rhythm disruptions
- Regular exposure to trauma
- A culture that sometimes discourages seeking help
Over time, this can lead to “allostatic load,” the wear and tear on the body’s stress systems (McEwen, 2007). The result is:
- Elevated cortisol for long periods
- Chronic inflammation
- Higher rates of burnout and metabolic dysfunction

Metabolic Consequences: The Path Toward Burnout
When the body is stuck in a state of chronic stress, this affects metabolism in many ways, including:
- Abdominal obesity
- Chronic fatigue
- Elevated blood pressure
- Increased blood sugar
- Poor cardiovascular health
First responders and veterans have statistically higher rates of metabolic syndrome, type 2 diabetes, and hypertension compared to the general public (Violanti et al., 2017).
How to Protect Metabolic Health
Here are research-backed strategies to help manage the stress response and protect your metabolism:
1. Prioritize Consistent, Restorative Sleep
Shift work can destroy circadian rhythm. Good sleep hygiene includes:
- Going to bed at the same time daily
- Blocking blue light before sleep
- Using a cool, quiet room
This helps regulate cortisol and allows for recovery (Medic et al., 2017).
2. Incorporate Regular Physical Activity
Exercise burns off excess adrenaline and lowers baseline cortisol over time. Recommended activities include:
- Resistance training
- Cardio (e.g., walking, cycling, swimming)
- Yoga or stretching
(Tsatsoulis & Fountoulakis, 2006)
3. Use Stress Reduction Techniques
Mindfulness, breathing exercises, prayer, and meditation all help to regulate stress hormones (Pascoe et al., 2017).
Pro tip: Peer support groups for first responders and veterans are also a powerful way to process trauma and build resilience. The Trauma Resiliency Protocol-Peer Rescue is a tool that will help reset the nervous system with a non narrative non clinical approach. Heal Here
4. Focus on Balanced Nutrition
Avoid processed sugars and ultra-refined carbs that spike blood sugar. Instead, choose:
- Lean proteins
- Vegetables and fruits
- Fiber-rich whole grains
- Healthy fats like olive oil or avocados
This supports stable blood sugar and reduces insulin resistance (Bergouignan et al., 2011).
5. Seek Professional Help
There is no shame in getting help. Trauma-informed therapy, peer programs, and community resources can all reset a dysregulated stress system.

Building a Culture of Resilience
Leaders in police, fire, EMS, and the military can help by:
- Providing stress-management education
- Encouraging peer support
- Creating time and space for recovery
- Destigmatizing mental health treatment
By doing so, agencies protect not only their personnel’s mental health but also their long-term metabolic and cardiovascular health.
Final Thoughts
The demands of military service and first responder work are inherently stressful, but that stress does not have to lead to chronic disease. Understanding cortisol and adrenaline, and how to regulate these hormones, can safeguard metabolic health and extend both quality of life and career performance.
For first responders and veterans, investing in your own well-being is a mission worth pursuing and if you would like to participate in a groundbreaking research study click the Human Performance Study below. Human Performance Study
References
Bergouignan, A., Latouche, C., Heywood, S., Grace, M. S., Reddy-Luthmoodoo, M., Natoli, A. K., … & O’Donoghue, G. (2011). Effect of exercise training on insulin resistance and plasma adiponectin levels in obese men. Metabolism, 60(4), 524–533. https://doi.org/10.1016/j.metabol.2010.04.011
Dimsdale, J. E. (2008). Psychological stress and cardiovascular disease. Journal of the American College of Cardiology, 51(13), 1237–1246. https://doi.org/10.1016/j.jacc.2007.12.024
Ferri, M., Davoli, M., Perucci, C. A., & Pasqualini, M. (2021). Substance abuse and trauma: Research challenges in first responders. Addictive Behaviors, 122, 107036. https://doi.org/10.1016/j.addbeh.2021.107036
Herman, J. P., McKlveen, J. M., Ghosal, S., Kopp, B., Wulsin, A., Makinson, R., … & Myers, B. (2016). Regulation of the hypothalamic-pituitary-adrenocortical stress response. Comprehensive Physiology, 6(2), 603–621. https://doi.org/10.1002/cphy.c150015
McEwen, B. S. (2007). Physiology and neurobiology of stress and adaptation: central role of the brain. Physiological Reviews, 87(3), 873–904. https://doi.org/10.1152/physrev.00041.2006
Medic, G., Wille, M., & Hemels, M. E. (2017). Short- and long-term health consequences of sleep disruption. Nature and Science of Sleep, 9, 151–161. https://doi.org/10.2147/NSS.S134864
Melamed, S., Shirom, A., Toker, S., Berliner, S., & Shapira, I. (2006). Burnout and risk of cardiovascular disease: evidence, possible causal paths, and promising research directions. Psychological Bulletin, 132(3), 327–353. https://doi.org/10.1037/0033-2909.132.3.327
Pascoe, M. C., Thompson, D. R., Jenkins, Z. M., & Ski, C. F. (2017). Mindfulness mediates the physiological markers of stress: Systematic review and meta-analysis. Journal of Psychiatric Research, 95, 156–178. https://doi.org/10.1016/j.jpsychires.2017.08.004
Rosmond, R. (2005). Role of stress in the pathogenesis of the metabolic syndrome. Psychoneuroendocrinology, 30(1), 1–10. https://doi.org/10.1016/j.psyneuen.2004.05.007
Sapolsky, R. M. (2004). Why zebras don’t get ulcers: An updated guide to stress, stress-related diseases, and coping (3rd ed.). New York, NY: Holt Paperbacks.
Tsatsoulis, A., & Fountoulakis, S. (2006). The protective role of exercise on stress system dysregulation and comorbidities. Annals of the New York Academy of Sciences, 1083(1), 196–213. https://doi.org/10.1196/annals.1367.020
Violanti, J. M., Charles, L. E., McCanlies, E., Hartley, T. A., Baughman, P., Andrew, M. E., … & Burchfiel, C. M. (2017). Police stressors and health: A state-of-the-art review. Policing: An International Journal, 40(4), 642–656. https://doi.org/10.1108/PIJPSM-06-2016-0097


